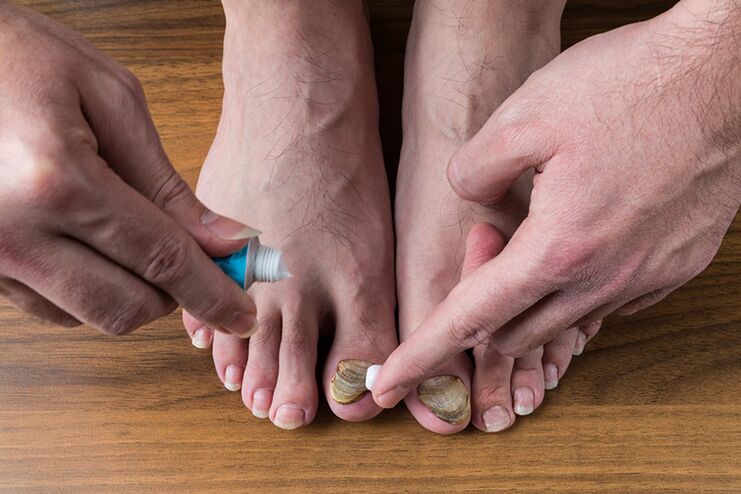
Nail fungus is one of the most common skin diseases. Fungal infections can affect the nail plate, nail bed, and surrounding skin. Fungal infections are more common on the toes, although the hands can also become infected. An invisible pathogen spreads to the feet on wet surfaces or through the air in bathrooms, saunas, swimming pools, gyms and other high-humidity locations.
Although nail fungus is statistically more common in older men with poor health, anyone can get it. Children often bring the disease with them from camp or sports clubs. Sometimes you may be infected by a relative in your home. To prevent serious complications, it is important to recognize the infection promptly and initiate treatment.
Types of toenail fungus
There are thousands of species of fungi that can inhabit a human being or coexist peacefully with him. Only a few of these cause onychomycosis or otherwise damage the nail plate.
If you're not sure what's causing the change in nail structure, see your doctor. Based on external signs, skin condition, and laboratory test results, specialists will be able to identify the causative agent.
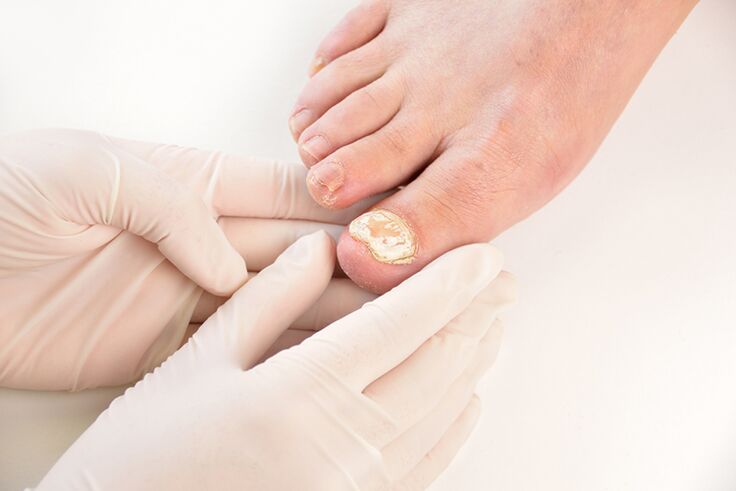
Dishes begin to be damaged when infected with one of the following fungi:
- dermatophytes. Common pests associated with chronic diseases of the skin, hair and nails. The pathological process develops against the background of a weakened immune system. If your immune defenses are working properly, the infection will be limited to a short-term, barely noticeable peeling of the skin. You can acquire spores in moist environments that help the fungus Trichophyton multiply rapidly. This dermatophyte occurs mainly on the thumb. In the early stages, the skin around the fingers is affected. You can also get other dermatophytes in a steamy sauna or in the bathroom of your own home. Trichophyton rubrum is initially visible only at the ends of the plates, but gradually captures the entire surface down to the roots. Infection is accompanied by stratification.
- Yeast. Infection of the skin of the hands or feet, which quickly develops protection against drug treatment. After infection, mushrooms like candida can linger on your skin or mucous membranes for years. Signs of the disease only appear when your immune system is weakened -- for example, in fall or early spring. The focus of infection develops on the roots. Nails quickly change color and become dull. The disease does not disappear without systemic treatment, but rarely enters an acute phase. The lesions may temporarily disappear as immunity builds up.
- moldFor serious systemic lesions, moldy fungi are often the culprit, and scientists have classified more than 40 of them. Mold biodistribution is so active that laboratory studies do not always give definitive results about the nature of the disease. As a result, the fungus has not been diagnosed in time, or it has been forcibly treated with various drugs for a long time. If you cannot find your medicine within six months, you run the risk of serious complications.
sign
In the first stages of infection, it is impossible to identify the fungus on its own. Only when the fungus reached a critical mass of living cells did the state of the nail plate change. Nails and skin colonize faster if your natural defenses are weak:
- Deterioration of health - weakened immunity due to nutritional deficiencies or imbalances, viral attacks or cold weather;
- The body does not have the resources to fight the disease;
- The nutrition of the nail bed is disturbed.
In the absence of all of these factors, the disease can still start, but neither you nor others will notice it.
Onychomycosis can gradually begin to develop if the fungus manages to break through the body's defenses and gain a foothold on the skin or nail plate. Affected areas will darken and pores will appear between layers. If left untreated, the board will start to delaminate.
Gradually, the entire nail surface may crack, cover with a cloudy coating, and then turn black. You can remove black nails with special plasters or other methods, but this will not protect you from recurrence of the fungus. As the nail plate slowly turns black, the spores penetrate deeper layers of the skin. Without treatment, new nails can grow over already diseased, deformed, or discolored nails.
There are several types of infections. They can be identified by the main characteristics indicated in the table.
view |
symptom |
|---|---|
Underarm shape |
In the distal phase, skin irritation rarely occurs. Changes can only be determined by the appearance of the nail plate. An early symptom of onychomycosis is gray or yellow streaks at the end of the nail. If this part of the nail becomes brittle or flakes and continues to turn black even after cutting the infected part, you need to see a doctor. A less obvious sign is slow growth of well-nourished nails. |
white surface mold |
A small white spot appears on the nail and does not cause discomfort. The skin is usually not peeling, red, or itchy. Cosmetic imperfections on the nails can appear and disappear without treatment. Other small defects form at the site of the lesion: tiny depressions on the plate, nodules. Symptoms of the disease usually appear after a prolonged stay in a humid environment. |
proximal subungual morphology |
The first symptom is a thickening of the base of the nail fold. The first stages of the disease usually go unnoticed because the affected area is small. The color of the pores changes - from white transparent to cloudy yellow, then to white. Affected nails grow very slowly, but do not crack or fall out. A few months after the color of the holes changed, the boards started peeling off quickly. |
Total destruction (advanced form of fungal disease of any kind). |
The color of the plates changes noticeably, the nails turn yellow. Nails look unpleasant, collapsed along their entire length. Behind the shed tissue, skin is visible where it would normally be closed. The skin around the infected finger becomes inflamed and red. Possible scabies and itching. |
How to Treat Toenail Fungus
The sooner the disease is caught, the easier it is to treat onychomycosis. This disease does not appear overnight. If you check your toes every time you shower, you'll notice unpleasant signs on your skin and nails long before your nails are damaged. Are there signs of infection? Then you need to see a doctor as soon as possible.
- A dermatologist will conduct laboratory examinations of the material on the deck, assess the stage of the lesions and choose a medication. Depending on the type of infection, your doctor may prescribe monotherapy or systemic treatment. In the latter case, you will have to continue taking the medicine or applying ointments to the skin for six months after recovery. This will ensure that there is no recurrence.
- A beautician can cover the affected plate with a medical varnish, choose a cream for inflamed skin, or perform nail removal. Cosmetic treatment does not eliminate the cause of the infection but makes conservative treatment more effective. Biological material destroyed by fungi is infectious. By removing the sloughed tissue, the cosmetologist removes the largest point of infection.
Many types of onychomycosis appear mild - white coating, brittle or slow-growing nails. For these types of lesions, topical treatments are appropriate. Doctors prescribe topical preparations - ointments, creams, gels - that do not transfer ingredients into the bloodstream. This treatment does not have unpleasant consequences in the form of allergic skin reactions or physical weakness. The drug acts on the focus of the infection, so recovery is faster.
Systemic treatment of fungal diseases is indicated in the following situations:
- large deformation along the entire length;
- cracks or creases;
- The process has spread to multiple nails and the skin on the fingers is contagious;
- damaged, infected nail roots;
- Appearance of large black or yellow areas;
- The board is layered to the bottom;
- fungus found on the skin;
- Quick fixes didn't help.
Systemic treatment begins with diagnosis. It is important to quickly identify the reason for starting targeted therapy. While taking your medicines, you must also take steps to improve your health. Your doctor may recommend staying home for the first week to prevent acute infections.
For complex treatment, two classes of drugs are chosen:
- to relieve symptoms. Onychomycosis and other forms of athlete's foot often cause skin irritation and itching. This robs an already weak body of strength.
- Drugs with cumulative effects. This type of fund doesn't jump right into action. The drug must enter the bloodstream through the skin or stomach and accumulate in sufficient quantities in the nail plate. After a few weeks, the fungus dies on its own.
potent antifungal
You can cure nail and skin fungus without leaving your home. But if you choose the wrong treatment, under the right conditions, the infection can grab your finger again. You should treat yourself only if you're staying home sick or temporarily unable to see your dermatologist for other reasons. In this case, it is worth trying home-friendly medicines:
- Imidazole topical cream. It treats onychomycosis, early forms of mycosis, and most fungal infections known to science. Suitable for treating nail plates and skin. One of the first and most popular methods: Quickly kills fungal colonies and prevents recurrence. It can be used at home without medical supervision: the drug has practically no contraindications.
- Antifungal agents for external use, belonging to the class of allylamines. It treats the consequences of onychomycosis and other forms of mycosis, is safe for the skin and is suitable for the treatment of children and pregnant women. This is a fast-acting cream: complex forms of the disease are treated within a few weeks. If deformation or white patches form again after a few months, the procedure must be repeated.
















