How to identify foot fungus
- In the earliest stages, patients will notice severe peeling of the skin, which is not completely eliminated even with standard foot treatments and the use of ointments;
- The itching gradually starts to bother you and gets worse every day and causes severe discomfort;
- Along with itching, there is a sour odor, which occurs when fungi appear on the skin; with a strong sweaty odor (increased sweating due to dysfunction of the subcutaneous glands);
- The color of the skin on the feet also changes, with the epithelial cells in the affected areas taking on an unnatural color: blue, green or even gray-black (in advanced cases).
important!The stage and type of fungus cannot be determined independently, so if you suffer from a skin disease, you must see an experienced specialist.
Why is foot fungus dangerous?
notes!Podiatry is characterized by fungal infections that are contagious, and because people often walk without shoes, sufferers put a large number of people at risk for infection.
- The disease transforms into a chronic form;
- decrease in immunity;
- Increased risk of other skin lesions.
- allergy;
- The rash spreads locally or regionally;
- Generalized skin lesions;
- Formation of papules, erythema, and eczema.
What causes foot fungus?
- decrease in immunity;
- Have vascular disease;
- Violation of hygiene rules.
- Diseases related to immune deficiencies;
- Rarely change socks and wear low-quality shoes;
- Going to public baths (without paying attention to personal hygiene);
- Onychomycosis;
- Increased sweating of the feet.
Is tinea pedis contagious?
important!Given how foot fungus spreads, you should also consider the risk of infection among people who come into contact with the patient, especially those who live with the patient.
How is foot fungus spread?

- Direct: foot contact with an infected surface, contact with a patient's feet, contact with an animal whose fur contains spores.
- Indirect: contact with personal belongings of patients with fungal diseases (socks, shoes, towels, etc. ), contact with care products of infected animals.
Types of foot fungus
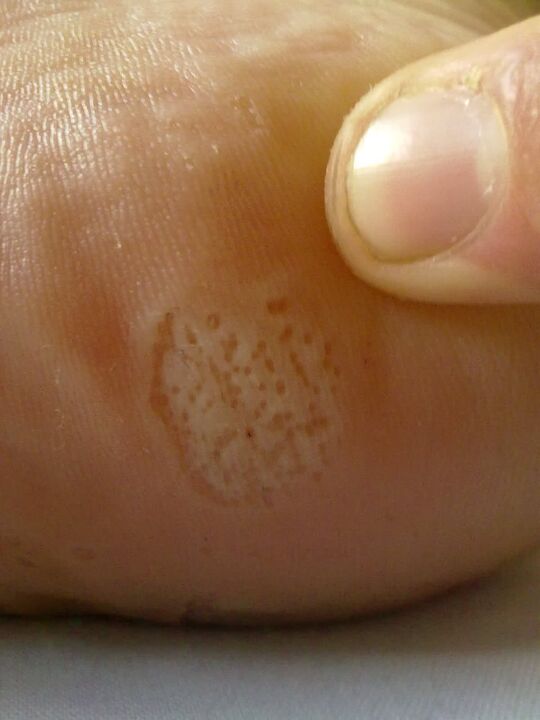
- Crossed fingers. Fungal diseases affect the skin between the toes. With this form, two stages can be distinguished: intertriginous and squamous. Most of the time, the infection becomes chronic because the area between the fingers is most favorable for the reproduction of fungal spores.
- soles of feet. The epithelial layer of the soles of the feet is affected by fungal diseases. It is characterized by severe keratinization, cracking and exfoliation of tissue.
- sweating disorder. The most painful form of foot fungus involves the formation of blisters and bubbles on the soles of the feet, which when the blisters burst, can lead to secondary infection.
- Deep mycosis. With deep mycosis, a large area of the foot is infected and the infection penetrates deep into the skin.
- Onychomycosis. This form may be a cause or consequence of dermatomycosis of the legs. When you have onychomycosis, the nail plates on your feet become infected.
interdigitated form
notes!In the case of infectious lesions of the feet, interdigital fungus of the feet in children is diagnosed in 70% of cases. Children move around a lot and spend a lot of time outside, often without shoes or socks.
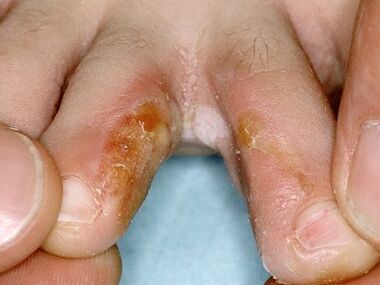
Stages and their manifestations
Early stage
How does the squamous hyperkeratosis stage manifest?
Sweating difficulty stage

How to Treat Foot Fungus
- medicinal;
- folk
Medication method
ointment
important!The effectiveness of topical medications is apparent in the first stages of treatment, however, in cases of severe foot lesions, the use of ointments alone may not be enough.
pill
important!Tablets are contraindicated during childhood, lactation and pregnancy.
traditional healing methods
notes!Folk remedies are not a substitute for medical treatment. Alternative medicine is only recommended as a complementary therapy.
vinegar and hydrogen peroxide
celandine juice

















